Traditional Chinese Herbal Medicine & the Nervous System
Adding Chinese herbal medicine to your Acupuncture treatment:
Herbal medicine has been used within Traditional Chinese Medicine (TCM) for thousands of years…longer than Acupuncture by far. Historically, formulas were designed to restore balance in individuals experiencing patterns of stress, agitation, anxiety, or sleep disruption.
TCM herbs can be a very gentle way to nourish the body back to a regulated state and is a very helpful addition to regular acupuncture treatments.
Stress as a Whole-Body Process
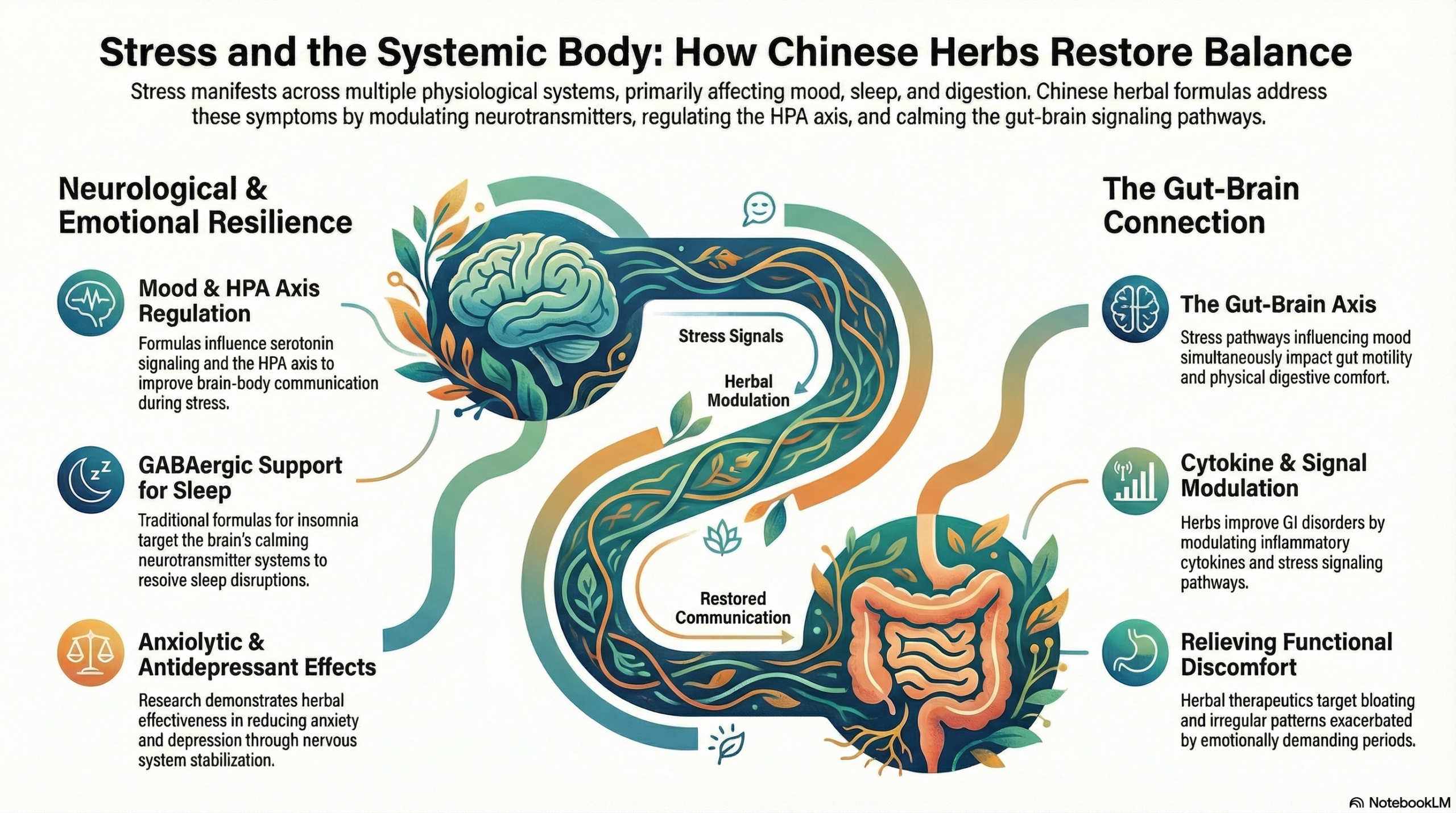
Chronic stress affects more than mood. It alters sleep architecture, digestive function, muscle tone, and hormonal rhythms. The hypothalamic–pituitary–adrenal (HPA) axis — one of the body’s primary stress regulation systems — can become dysregulated over time.
Think of the HPA axis as your internal thermostat for stress. When it’s working properly, it rises and falls in response to real demands. When it’s dysregulated, it may stay elevated too long or respond too strongly to small triggers.
Research over the past several years suggests certain traditional Chinese herbal formulas may help modulate this stress thermostat.
Herbal Formulas and Anxiety
Several classical formulas used historically for irritability, emotional tension, and stress have been studied in modern trials.
For example, modified versions of Xiao Yao San, a traditional formula used for stress-related mood disturbance, have demonstrated anxiolytic (anxiety reducing) and antidepressant effects in both animal models and human studies. Recent research suggests this formula may influence serotonin signaling and regulate HPA axis activity (Zhang et al., 2018; Liu et al., 2020).
In simple terms, certain herbs appear to help the brain communicate more smoothly with the body during stress.
Patients often describe this effect not as feeling “drugged,” but as feeling less reactive — as though their emotional responses have more space around them.
Herbal Medicine and Sleep
Sleep disruption under stress often reflects both nervous system activation and hormonal imbalance. Some traditional formulas used for insomnia — such as those containing Suan Zao Ren (Ziziphus jujuba seed) — have been studied for their effects on GABAergic activity, one of the brain’s calming neurotransmitter systems.
A 2020 systematic review found evidence supporting the use of traditional Chinese herbal formulas for improving sleep quality and reducing insomnia severity compared with placebo (Yeung et al., 2020). More recent trials suggest improvements in sleep latency and sleep duration through modulation of stress-related neurochemistry (Wang et al., 2022).
If anxiety and insomnia feel like a cycle — one worsening the other — herbs may help soften both sides of that common issue.
Digestive Symptoms and Stress
Stress frequently presents in the digestive system. Bloating, irregular bowel patterns, and functional discomfort often worsen during emotionally demanding periods.
From a modern perspective, this is closely tied to the gut–brain axis. The same stress pathways that influence mood also influence gut motility and inflammation.
Recent research examining traditional herbal formulas for functional gastrointestinal disorders suggests modulation of inflammatory cytokines and stress signaling pathways may contribute to symptom improvement (Chen et al., 2019; Li et al., 2021).
An analogy I often use is this: if the nervous system is a communication highway, stress creates traffic congestion. Herbal formulas, when chosen appropriately, may help reduce that congestion — allowing signals to move more smoothly.
How Herbal Medicine Differs from Symptom Suppression
Western pharmaceuticals often act quickly and specifically on one receptor system. Herbal formulas tend to work more gradually and across multiple systems at once.
Rather than forcing a single pathway, formulas are typically designed to nudge several regulatory systems simultaneously — nervous, hormonal, and digestive.
This multi-system effect is one reason they are traditionally prescribed as combinations rather than single isolated compounds.
It is also why individual assessment matters. The same symptom — insomnia, for example — may arise from different underlying stress patterns in different people.
Integration, Not Replacement
Traditional Chinese herbal medicine is not meant to replace necessary medical care. It can, however, serve as a complementary strategy for individuals seeking a regulatory approach to stress, anxiety, and insomnia.
When appropriately prescribed and monitored, herbal formulas may support nervous system flexibility, improve sleep stability, and reduce stress reactivity over time.
The goal is not simply to quiet symptoms.
The goal is to help the system recalibrate.
Getting Help With Drew
If your nervous system has been in overdrive for some time, that does not mean this is your permanent state. Adaptability can be rebuilt. If you’re experiencing ongoing stress, anxiety, insomnia, or stress-related digestive symptoms, I encourage you to book an appointment.
Together, we can evaluate how your system is functioning and create a structured plan to help it regain flexibility and resilience.
References
Chen, H., et al. (2019). Traditional Chinese herbal medicine for functional gastrointestinal disorders: Mechanisms and clinical evidence. Journal of Ethnopharmacology.
Liu, Y., et al. (2020). Xiao Yao San and modulation of HPA axis in stress-related disorders. Frontiers in Pharmacology.
Wang, L., et al. (2022). Effects of traditional Chinese herbal formulas on insomnia: A randomized controlled study. Evidence-Based Complementary and Alternative Medicine.
Yeung, W. F., et al. (2020). Herbal medicine for insomnia: A systematic review and meta-analysis. Sleep Medicine Reviews.
Zhang, Y., et al. (2018). Mechanisms of Xiao Yao San in anxiety and depression models. Pharmacological Research.

