Understanding Digestion and Stress: When the Gut Feels What the Mind Carries
Digestive symptoms are among the most common — and most misunderstood — effects of chronic stress.
Bloating. Irregular bowel movements. Stomach discomfort before meetings. Loss of appetite during stressful situation. Or the opposite — stress-driven cravings and bowel urgency.
For many people, digestive symptoms seem unpredictable.
In reality, they are often deeply connected to the nervous system.
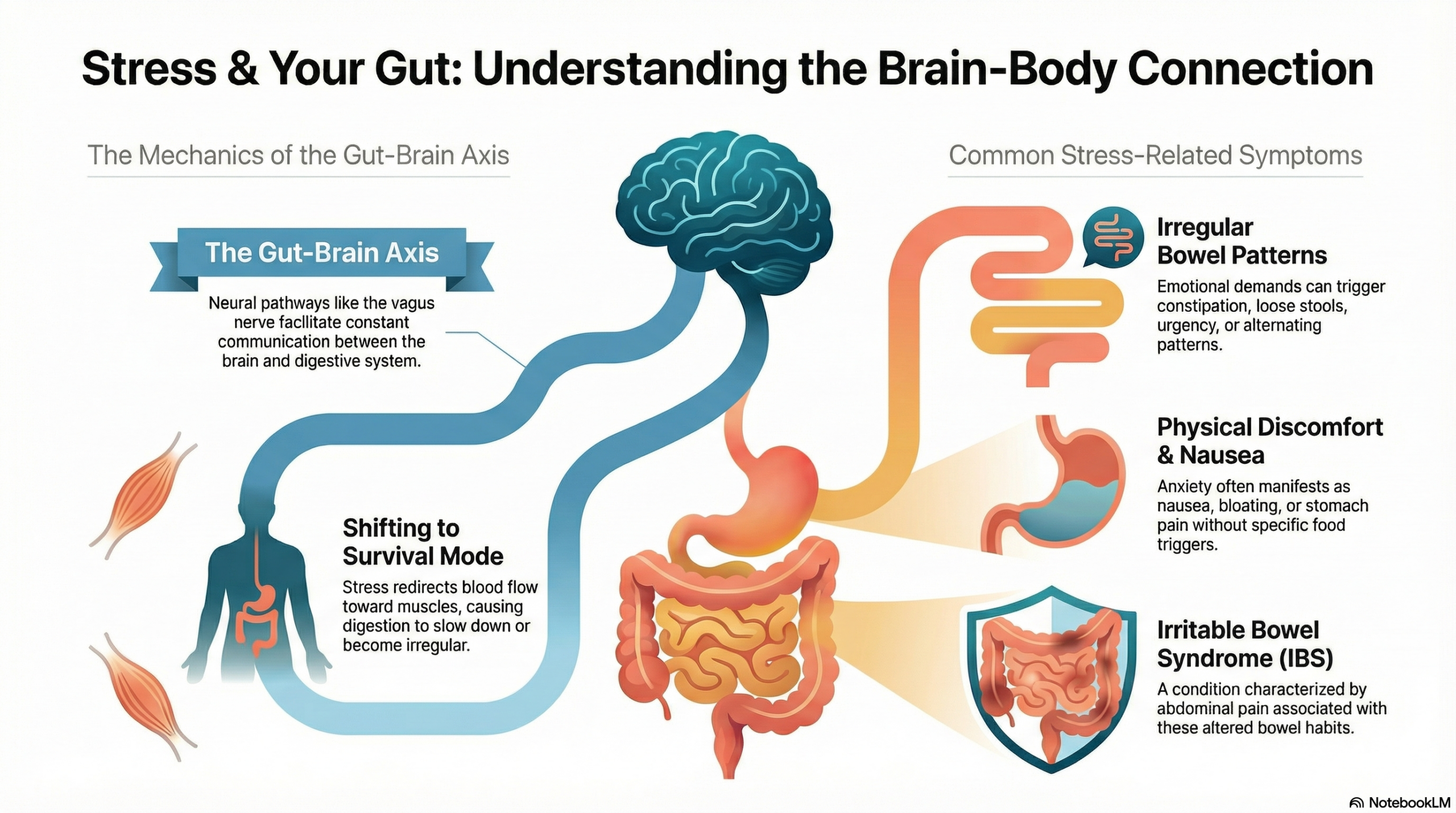
The Gut–Brain Connection
The gut and brain are in constant communication.
They are connected through neural pathways (including the vagus nerve), immune signaling, and hormonal systems. This network is often referred to as the gut–brain axis.
When you feel stressed, your digestive system knows.
If the body perceives a threat — whether physical or emotional — it shifts into survival mode. Blood flow is redirected toward muscles. Digestion slows or becomes irregular. Motility changes. Sensitivity increases.
This makes sense evolutionarily. If you were running from danger, digestion would not be a priority.
The problem arises when this state becomes chronic. Often leading to a fear of being away from the nearest bathroom and resulting in you missing out on the enjoyable things in life – going to a concert, having lunch with friends or taking a vacation.
Common Stress-Related Digestive Symptoms
Stress can affect digestion in different ways. You may notice:
- Bloating that worsens during stressful days
- Constipation during emotionally demanding weeks
- Loose stools or urgency before important events
- Stomach discomfort without clear food triggers
- Alternating bowel patterns (constipation then diarrhea)
- Nausea when anxious
Some people are diagnosed with Irritable Bowel Syndrome (IBS), which is characterized by abdominal pain associated with altered bowel habits. Stress does not cause IBS on its own, but it is a well-recognized trigger for symptom flare-ups.
In fact, many individuals with IBS report that emotional stress reliably worsens their digestive symptoms.
This does not mean the symptoms are “in your head.”
It means your gut is responsive to your nervous system.
Why the Gut Becomes More Sensitive
Under chronic stress, two key changes often occur:
- Motility shifts — the speed at which food moves through the digestive tract can increase or decrease.
- Visceral sensitivity increases — meaning normal digestive activity may feel more uncomfortable or noticeable.
An analogy I often use is this: imagine turning up the sensitivity dial on a microphone. Sounds that were previously subtle now feel amplified.
Stress can amplify internal sensations in a similar way.
Research over the past several years has shown that stress influences inflammatory markers, gut permeability, and microbiome composition (Moloney et al., 2019; Foster et al., 2021). While the science continues to evolve, it supports what many people already experience: emotional stress has measurable digestive consequences.
The Vicious Cycle
Digestive symptoms themselves can then increase stress.
You may begin to anticipate discomfort before social events. Or worry about bathroom access. Or restrict foods out of fear.
This anticipatory stress further activates the nervous system, which can worsen digestive sensitivity.
Over time, digestion may feel unreliable.
Long-Term Effects of Ongoing Stress on Digestion
When stress remains elevated for long periods, digestive disturbances can become persistent.
You may notice:
- More frequent flare-ups
- Reduced tolerance for certain foods
- Increased abdominal tension
- Fatigue related to poor nutrient absorption
- Heightened food-related anxiety
Again, this does not mean permanent damage has occurred.
It means the nervous system has been under sustained demand.
A Reassuring Perspective
The digestive system is highly adaptive. When the nervous system begins to stabilize, digestion often follows.
Many patients are surprised that as sleep improves and anxiety decreases, bloating lessens. Bowel movements become more predictable. Abdominal discomfort softens.
This doesn’t require extreme dietary restriction or perfection. It requires regulation.
If you are experiencing digestive symptoms that seem to worsen with stress, fluctuate unpredictably, or coexist with anxiety or sleep disruption, it may be helpful to address the nervous system alongside dietary factors.
Digestive discomfort is not always a food problem alone. Sometimes, it’s a stress pattern expressed through the gut.
If ongoing digestive symptoms have been affecting your quality of life, booking an appointment can help clarify what may be contributing and how to approach it in a structured way.
Your gut is not working against you. It is responding to signals.
And those signals can change.
Getting Help With Drew
If your nervous system has been in overdrive for some time, that does not mean this is your permanent state. Adaptability can be rebuilt. If you’re experiencing ongoing stress, anxiety, insomnia, or stress-related digestive symptoms, I encourage you to book an appointment.
Together, we can evaluate how your system is functioning and create a structured plan to help it regain flexibility and resilience.